Could Low Testosterone Increase the Risk of Varicose Veins in Men?

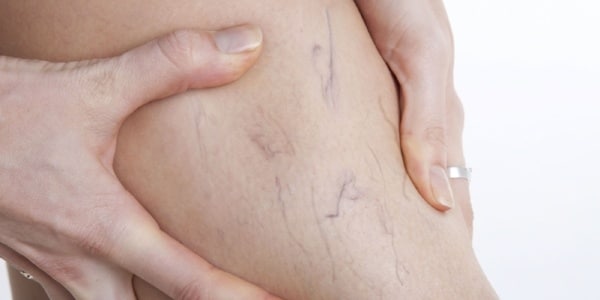
It’s a common misconception only women suffer from varicose veins, however, it is estimated that somewhere between 15% and 45% of men will develop varicose veins or venous insufficiency at some point in their lives. The exact number is unknown, primarily because a significant number of men do not seek treatment for vein disorders.
There are several factors that contribute to varicose vein formation; genetics, age, diet, exercise, stress, and weight are all important to vein health. But gender is also considered a risk factor and there are some indications that our “sex hormones” may be the culprit - particularly estrogen.
Estrogen in Men? Definitely!
While women synthesize most of their estrogen in their ovaries and other reproductive tissues, men produce estrogen through a process involving an enzyme called aromatase. Aromatase is found in many tissues including gonads, brain, adipose tissue, blood vessels, skin, and bone. Aging men sometimes have too much aromatase activity, which causes their testosterone to convert to excess estradiol, the predominant form of estrogen.
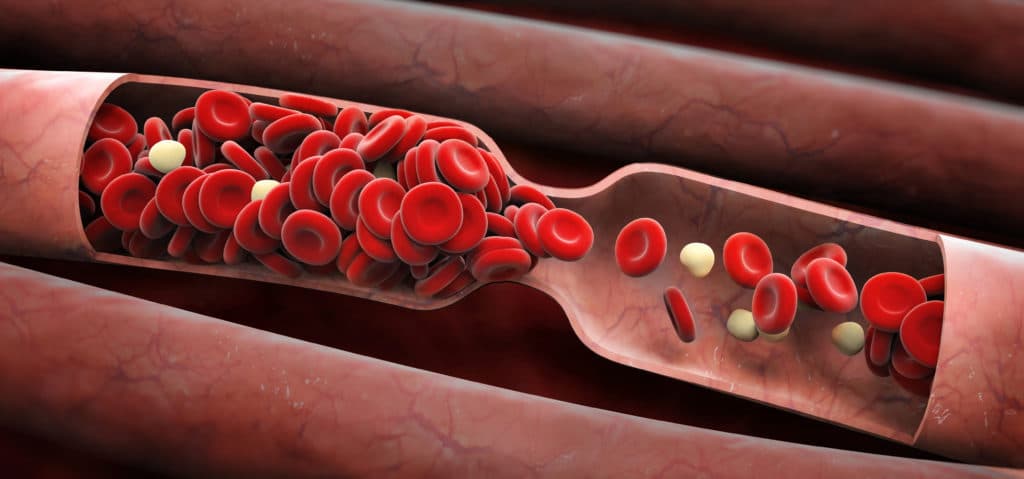
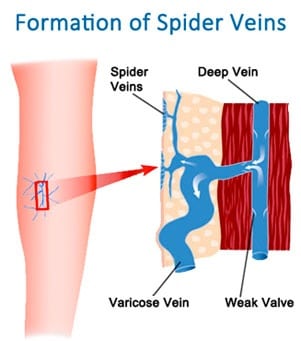
Estradiol is a known contributor to varicose vein development in pregnant women; it shrinks and impairs the function of venous valve flaps, breaks down the integrity of venous walls, and causes blood vessels to dilate, or get wider. So what does estrogen have to do with varicose veins in men? It could be a lot!
While it is too small to be clinically significant, a study published by researchers at the Universitat Leipzig in Germany noted that all of the men in their study with varicose veins had higher levels of estradiol and lower levels of testosterone (low T) compared to the men with healthy veins. What this shows is that estradiol alone is not the culprit, rather the ratio of estradiol to testosterone appears to be the determining factor.
As men age, testosterone levels naturally decline. Where a younger man’s testosterone to estrogen levels might naturally be 50:1, an older man might experience a ratio of 8:1. What the science seems to suggest is that when the ratio of estrogen to testosterone is out of whack, men are at higher risk for developing vein disorders.
Concerned About Your Vein Health?Click Here to Download a Self Assessment |
Restoring Hormone Balance is Good for Vein Health
The hormonal system helps to govern all aspects of the bodies’ functions. Its interconnectedness is complex; its balance is somewhat delicate and can be easily thrown off track. We are bombarded by stories about potential hormone disrupters and estrogen mimickers that some fear, are messing up these complex systems. Regardless of whether this is true, there are many lifestyle choices that men can make to help maintain—or restore—hormonal balance and improve their vein health.
- Maintain a healthy weight. Obesity is a significant risk factor, both for overproduction of estrogens and for varicose vein formation. Not only do the extra pounds increase strain on the vascular system, but also fat cells are particularly rich in the enzyme aromatase. The more aromatase in the system, the more testosterone will be converted to estradiol.
- Manage your stress levels. Cortisol, the hormone associated with the “fight or flight” response, increases when stress levels are high. High cortisol levels inhibit testosterone production.
- Get good quality sleep. Most testosterone is produced when we sleep. Actually, a lot of important things happen only when we are sleeping. Plus, sleep is just awesome.
- Nourish your body. It is important to eat a wide variety of whole foods in order to get the building blocks required for good hormone production and balance.
- Exercise the right amount. Moderation in all things. Studies have found that men who exercise a LOT have lower testosterone levels than their counterparts who exercise a moderate amount.
Men who develop varicose veins should consult with a qualified vein specialist to determine whether their vascular system is compromised, and what can be done to improve venous blood flow back to the heart.
Tempe-based vein specialist, Jilanne Rose of Advanced Vein Institute of Arizona, has noticed that men tend to wait until their veins get painful—or worse—before seeking treatment. Because of this tendency, she encourages everyone to look out for the vascular health of the men—and the women—in their lives.
And these days, Jilanne adds, it is easier than ever to improve vascular health. Vein treatments are less invasive, less painful, less expensive and more successful than they have ever been. Simply make an appointment with a qualified vein specialist who can precisely determine the health of your lower extremity veins, and help you make informed decisions about what treatment (if any) is right for you.
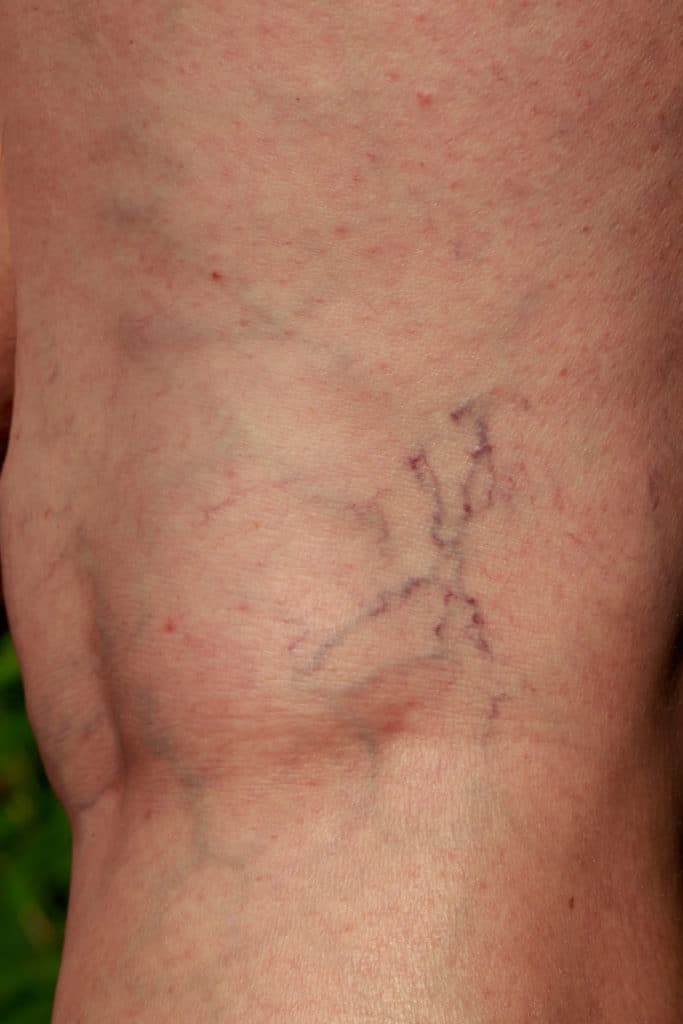
Question: I have spider veins on my legs and they really hurt to the touch. Can that be dangerous to my health? Answer: In the large picture, pain associated with spider veins is not life threatening. It would be worthwhile to have an evaluation by a qualified provider to see if these spider veins are…
Read MoreI am scheduled for a right leg radiofrequency ablation. I have venous insufficiency in the saphenous vein and have had a blood clot before. Question: In 2006, I underwent an artificial lumbar disk implant. This failed causing artificial disk to move into the spine. While surgeon removed the artificial disk implant, he nicked the liac…
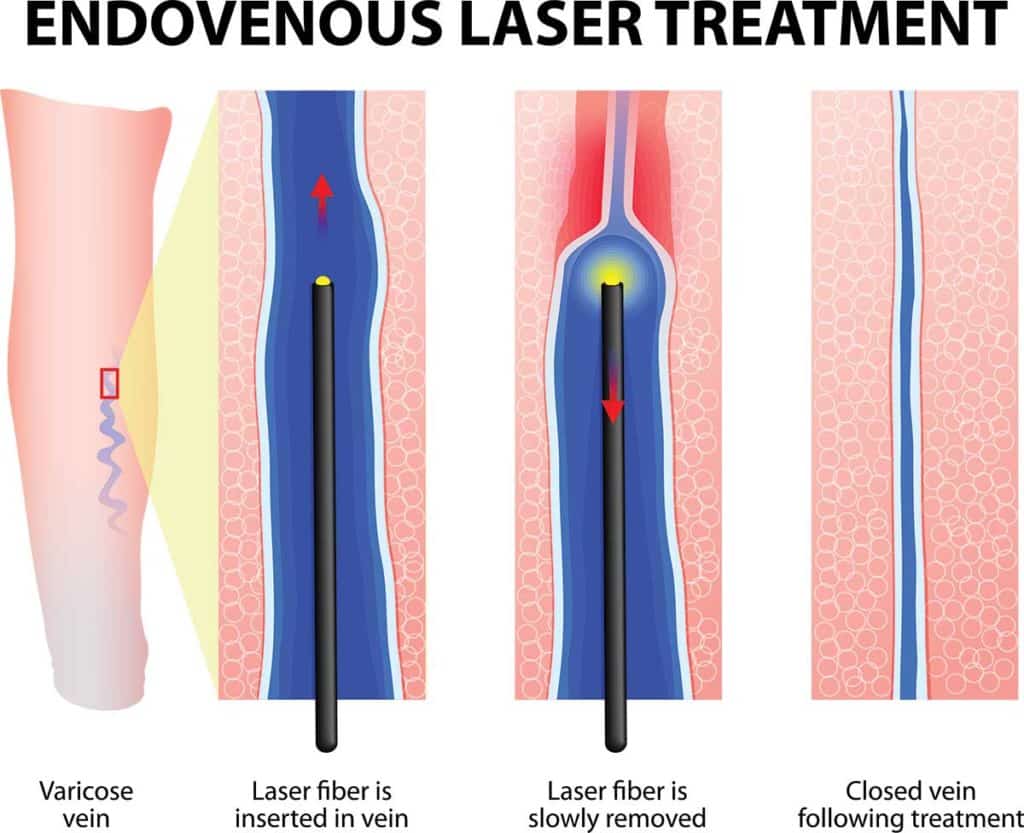
Read MoreMy doctor said my vein is too large to have sclerotherapy performed first, is this true? Question: I have a few visible spider veins on my lower leg that I want treated with foam sclerotherapy. However, the doctor wants me to do endovenous laser treatment before the sclerotherapy. According to him, my vein is way…
Read MoreI’m having the same pain that I had before my ablation procedure, except it is in a different new location. How long will this go on? Question: It’s been 2 months since my GSV endovenous laser ablation procedure. I have the same pain that I had before the procedure, except it’s in a new location.…
Read MoreI recently had the VNUS procedure done (both legs, multiple veins). Is it normal to have open, circular wound with redness and slight weepiness? Question: All of the other areas are healing nicely, but the area on my shin (a bit off center) has a much larger wound. It has been quite red in the…
Read MoreQuestion: How big of a size do compression stockings come in? Answer: Compression socks should be comfortable and supportive. If the stockings are making your symptoms worse, it is likely that they do not fit you correctly. There are numerous companies that make standard sized compression stockings. Some make 7 to 8 different sizes. Additionally,…
Read MoreQuestion: WHAT CAN I DO TO GET RID OF MY VARICOSE VEINS? Answer: There are numerous options to treat varicose veins. Some are considered medically necessary, while others are strictly cosmetic. Larger veins are treated in a myriad of ways depending on the provider you consult with and their proficiency in a given intervention. The…
Read MoreQuestion: I knelt down the other day and injured the large varicose vein over my knee. It bruised quickly and felt very sore, so I put a pressure bandage on it. Since then, the vein bruise has spread and is now about 12″ up my thigh. It is very red, and I’m not sure what…
Read MoreQuestion: What treatment options are available for my CVI? I can’t sit or stand in one place and I have heavy, aching legs all of the time. I started to have achy, heavy leg feelings about a month after I sprained my right ankle and scratched my left knee last April. I was diagnosed with…
Read MoreQuestion: During the EVLT laser procedure I really didn’t feel well, especially when the laser was on. I felt dizzy and the smell of “burning” freaked me out. Even after I was done, it took me couple hours to feel normal again. Is that normal? Answer: The “odor” and sometimes a taste is normal during…
Read More